While the pandemic has caused illness and death, decimated livelihoods and disrupted the daily lives of billions across the globe, its impacts are felt the hardest by the world’s most vulnerable people. Last year, the Efficiency for Access Coalition (where CLASP is Co-Secretariat) published an article exploring the implications of the pandemic on off-grid communities in sub-Saharan Africa and South Asia, and how solar technologies can bolster these communities’ resiliency to a global shock, like COVID-19. As a follow-up, the Coalition partnered with SolarAid to explore practical interventions for off-grid medical service provision in Malawi and Zambia.
Below, we’ll discuss these efforts, share the perspectives of healthcare staff and patients who have benefited from them, and explore how installing solar systems in rural health facilities can drastically improve the quality of care for patients across sub-Saharan Africa and in other emerging markets.
OFF-GRID APPROPRIATE APPLIANCES: THE MISSING LINK IN CLINIC ELECTRIFICATION EFFORTS
“For nurses on night duty, when you have a labour without lighting you will need to use phone torches, [but] the light is not enough,” said Marianne Mwale, a laboratory technician at St. Paul’s Mission Rural Health Centre in Zambia. “Maybe the woman will need a suture — how do you do that without enough light?”
The problem she described is distressingly widespread. As many as 59% of healthcare facilities in low- and middle-income countries lack reliable electricity. And in sub-Saharan Africa, nearly 25% of all healthcare facilities have no energy access at all. Without energy, clinicians cannot utilize basic diagnostic tools, maintain inventories of critical medicines and vaccines, or access information relevant to patient care. As a result, patients suffer: Mothers give birth in the dark, babies are born without neonatal warmers and preventative care for a wide range of treatable conditions is unavailable.
Though there are a number of clinic electrification initiatives currently aiming to address this, they often focus on the energy system itself, without equivalent consideration of the specialized medical equipment required to deliver health services. Few commercially available medical devices are designed to perform in harsh environments and with a limited energy supply, as medical device suppliers design most of their products for hospitals in Europe, North America or East Asia. Partially due to this mismatch, the WHO estimates that 70% of complex medical devices in the Global South do not function and remain unused.
SOLARAID PILOTS ‘PLUG AND PLAY’ SOLAR-POWERED MEDICAL DEVICES IN MALAWI
In Malawi, rural health facilities are struggling to provide basic healthcare due to the lack of reliable electricity. Where electricity is extremely limited, the ability to turn on a light or use a simple device, like an infrared thermometer, can save lives.
This year, SolarAid partnered with Malawi’s Ministry of Health to equip rural health facilities with solar technologies that are easy to use, install and maintain, designed to have an immediate and long-lasting impact. Prior to launching the project, our team at SolarAid conducted a workshop with the Ministry to identify the specific needs for power and equipment within different tiers of healthcare, from rural off-grid health centers to larger facilities connected to a weak or unreliable grid. Based on this assessment, we introduced plug-and-play systems, or smaller solar systems coupled with lights and batteries that can power appliances with a USB connection. Together, we identified the most relevant technologies and selected 20 sites to deploy the systems.
Early feedback from health professionals at the sites has been positive. “With this solar lighting, patients think we are connected to the electricity grid. It would be good if these can be brought to health clinics across the country,” said Angela Mbewe, a nurse at the Chadza Health Centre in Mitundu.
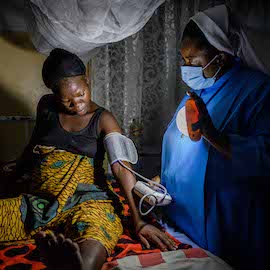
While relatively small solar systems cannot generate the electricity needed to power large hospitals, they can be rapidly deployed across rural healthcare facilities to generate enough electricity to power a wide range of critical smaller medical appliances. Some of the technologies powered in SolarAid’s pilot include pulse oximeters, foetal dopplers, infrared thermometers and digital blood pressure monitors – not to mention lighting.
Simply facilitating consistent lighting can significantly impact staff morale and increase productivity, especially during the night shift. “Less staff are willing to work in the darkness,” explained Eddie Kwaitana, a Health Officer at Mzuzu Central Hospital in Mzuzu. “With the solar lights, quality and quantity of service delivery will increase since more workers will be willing to work.”
POWERING HEALTHCARE IN ZAMBIA
SolarAid partnered with the Churches Health Association of Zambia in September 2020 to install solar home systems in 10 rural health facilities, along with solar chargeable medical equipment — like the systems piloted in Malawi. SolarAid has already installed the systems and conducted follow-up visits at three of the clinics, receiving widespread positive feedback from health facility staff.
“It has improved our work. The foetal doppler is faster and louder, you are able to get the foetal heart rate clearer… The patients feel nice when we use the foetal doppler — at least now, they are able to hear the heartbeat,” said Mercy Namwinga, a nurse at the Zambia Helpers Society Hospital in Chilanga District.
Early feedback from patients has also been positive. For instance, expectant mothers say they are now able to walk around maternity wards at night without the fear of bumping their bellies into objects.
“During my first pregnancy, I had to come with a torch for delivery in the event that the electricity went,” explained Olivia Chivita, a patient at Chipembi Rural Health Centre. “Now I no longer have to worry about that because the solar lighting is sufficient. It was hard for the medical attendants to see properly during the delivery with just a torch.”
To ensure that the solar systems remain operational in the long term, SolarAid enabled remote monitoring technology. As a result, the team at headquarters in the capital, Lusaka, is able to address technical issues and troubleshoot over the phone, as well as track how much power is consumed at the clinics.
SCALING SOLAR SOLUTIONS FOR UNDER-ELECTRIFIED RURAL HEALTH CLINICS
Through these pilots, SolarAid aims to demonstrate that it is possible to equip rural health facilities with solar solutions that can drastically improve the quality of care almost immediately. Given the early success of these efforts, the approach seems to have the potential to scale: The growing network of solar companies across sub-Saharan Africa is well-positioned to support improved health service delivery for millions across the continent.
However, financial barriers limit the scale-up of solar-powered medical devices. “Plug-and-play systems are available at a fraction of the cost of traditional solar systems, making them a cost-effective solution, explained John Keane, CEO of SolarAid. “But as we plan to scale up these innovations across Zambia and Malawi, more support will be needed.”
To that end, donors and investors must provide funding that is specifically dedicated to catalyzing innovations and building markets for high-priority medical equipment.
Dedicated R&D funding, as well as competitions and innovation prizes, can help identify early-stage market leaders like SolarAid. Funding can also break down silos between energy and health stakeholders and encourage new players, especially those already integrated in local markets, to engage with the medical equipment space.
Off-grid facilities are not the only beneficiaries of solar technology. Even at grid-connected clinics, electricity is often unreliable and power outages can be debilitating. Access to solar-powered appliances enables staff to continue working through blackouts: Healthcare workers can attend to emergencies, babies can be delivered safely and laboratory technologists are able to continue their work.
Efficiency for Access recently released a research brief presenting a preliminary assessment of the technical and commercial barriers to the large-scale deployment of medical equipment in off/weak-grid clinics. The brief includes a set of actionable recommendations for health and energy sector stakeholders to begin addressing these barriers, urging swift action to ensure quality health service delivery for vulnerable communities around the world.